 
There was no interaction between the treatment and varying impact of POAF. Early, late, or any POAF was not significantly associated with risk for major bleeding. Sometimes a person may have episodes of both atrial flutter and atrial fibrillation. People with atrial flutter have a heart rhythm that's more organized and less chaotic than that of atrial fibrillation. After adjustment, early POAF was not associated with increased 2-year risk for the composite outcome (hazard ratio, 1.10 95% confidence interval, 0.64-1.91 p = 0.72), but late (HR, 8.90 95% CI, 5.03-15.74, p < 0.0001) and any (HR, 2.39 95% CI, 1.45-3.94 p = 0.0006) POAF were. Atrial flutter is similar to atrial fibrillation, a common disorder that causes the heart to beat in irregular patterns. LAV and SAVR were independently associated with increased risk for early and any POAF. 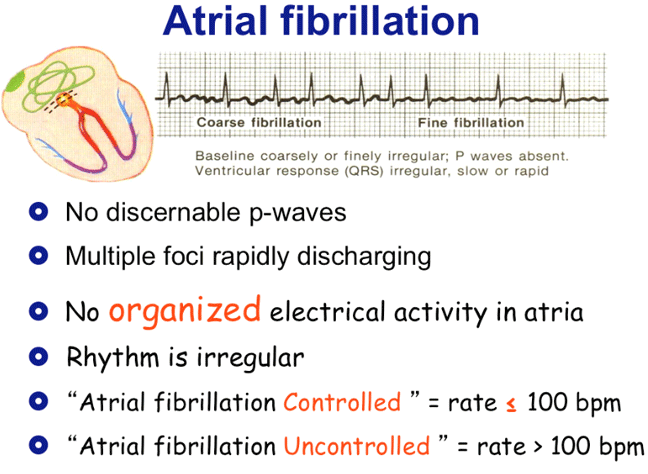
Within 1 year of the index procedure, any POAF was detected in 12.3% (n = 196), with 44.5% occurring after SAVR and 8.0% after TAVR (p < 0.0001). After discharge, late POAF occurred in 7.0% (n = 55) and again, significantly more frequently following SAVR (10.4% vs. 4.3%, p < 0.0001), although by the time of hospital discharge, early POAF had resolved in 31.9% of those in the SAVR group. Early POAF occurred in 19.5% (n = 152) and occurred significantly more frequently after SAVR than TAVR (36.6% vs. Of 781 patients included in the analysis, 366 underwent SAVR and 415 TAVR. Median follow-up was 2.1 years (interquartile range, 2.01-2.45 years). Multivariable Cox proportional hazards regression analysis was used to examine the association between POAF and adverse clinical outcomes. Logistic regression was used to predict early, late, and any POAF with a model adjusting for age, sex, history of diabetes, history of hypertension, history of congestive heart failure, history of stroke or transient ischemic attack, body mass index, baseline hemoglobin, creatinine clearance, left ventricular ejection fraction, left atrial volume (LAV), and treatment modality. 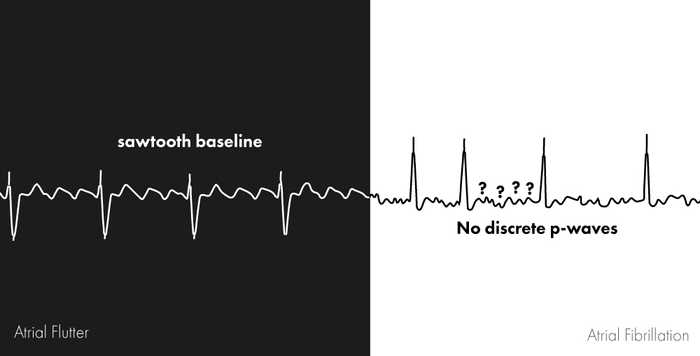
Secondary endpoints were rehospitalization for procedure- or device-related adverse events or heart failure, all-cause death, cardiovascular death, stroke, and major bleeding.Īnalysis was performed in the as-treated population. Atrial Flutter is a less severe heart condition than Afib. The primary endpoint was a composite of all-cause mortality, stroke, or rehospitalization at 2 years. Atrial flutter is a heart condition in which the rhythm of the heart is abnormal and irregular wherein Atrial Fibrillation is a condition when the heart beats at a very fast pace, the rhythm is normal but the pace is very fast. Those with pre-existing AF and those who did not undergo AVR were excluded. Patients who experienced POAF at any time following the index procedure and up to 1 year later were grouped into: 1) early, 2) late, and 3) any POAF. This is an analysis from the PARTNER 3 trial, a multicenter, prospective, randomized trial examining SAVR versus TAVR with a balloon-expandable valve in patients with severe aortic stenosis at low surgical risk for mortality from SAVR. 
0 Comments
Leave a Reply. |
 RSS Feed
RSS Feed
